Understanding Health Equity: Why Where You Live Determines How You Live
Health is often described as a matter of personal choice in America, they tell people to eat well, exercise, and visit the doctor regularly. But for millions of people, health outcomes are shaped long before making those choices are even possible. The truth is that where you live can significantly influence how long you live, the diseases you may face, and the care you can access. Health equity is a concept gaining more attention in public health, policy, and community development and understanding it requires looking beyond hospitals and clinics and examining the broader systems that shape everyday life.
Health equity refers to the idea that everyone should have a fair and just opportunity to maintain their best possible health. Achieving this goal requires removing barriers such as poverty, discrimination, and unequal access to education and healthcare.
According to the Centers for Disease Control and Prevention, social determinants of health are the nonmedical factors that influence health outcomes. This includes the conditions in which people are born, grow, work, live, and age in.
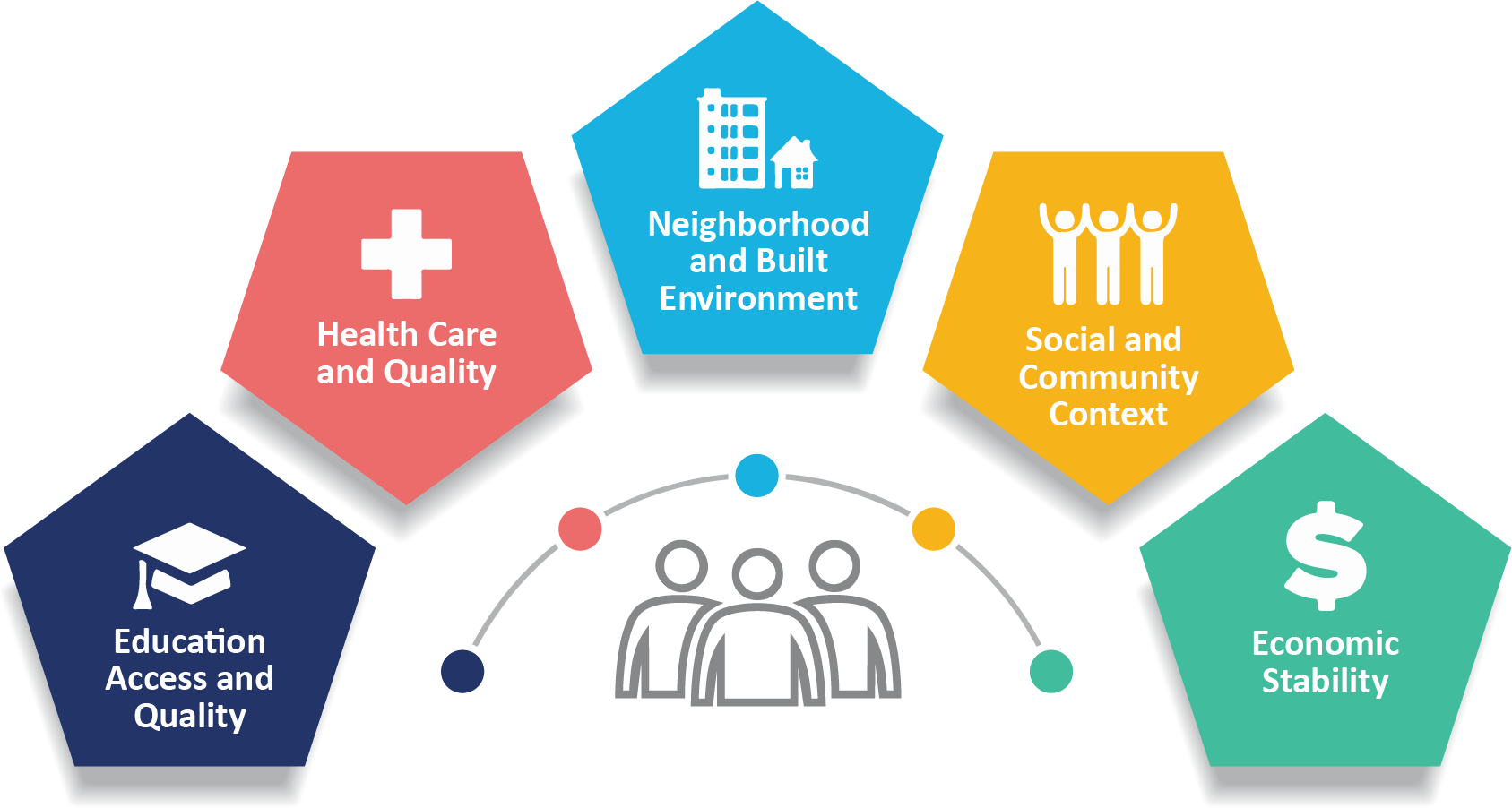
These factors include:
Economic stability
Education access and quality
Healthcare access and quality
Neighborhood and upbringing environment
Social and community factors
Together, these conditions shape daily life and ultimately determine whether individuals and communities have the opportunity to live healthy lives.
Why Your Zip Code Can Matter More Than Your Genetic Code
Research consistently shows that location plays a powerful role in health outcomes. In many cases, a person’s zip code can predict health risks just as much or more accurately than genetics. For example, communities with limited access to grocery stores often become “food deserts”, where residents rely on convenience stores or fast food. This lack of access to healthy food can increase the risk of obesity, diabetes, and heart disease. Similarly, neighborhoods with higher pollution levels may expose residents to environmental hazards that increase asthma or respiratory illness.
These disparities occur because social determinants shape both opportunities and risks in everyday life.
Economic Stability factors such as income and employment affect a family’s ability to afford nutritious food, stable housing, transportation, and healthcare. Economic instability is linked to higher stress levels and increased rates of chronic disease.
Education influences health literacy, job opportunities, and access to resources. Individuals with higher levels of education tend to live longer and experience better overall health and health care.
Healthcare Access varies widely between communities. In rural areas, for instance, physician shortages make it difficult for residents to receive regular check ups.
Neighborhood Environments such as housing quality, safety, air quality, and transportation all influence physical and mental health. Communities with safe parks and walkable infrastructure promote healthier lifestyles.
Social Factors like strong community networks, supportive relationships, and access to mentorship or social services can improve mental health and resilience.
When these factors combine negatively, they create health inequities, avoidable differences in health outcomes between populations.
Health Disparities in Underserved Communities
Health inequities are not distributed randomly. In the United States, low-income communities and communities of color often face greater exposure to harmful social determinants.
For example:
Higher rates of chronic disease such as diabetes and hypertension.
Lower life expectancy in economically disadvantaged neighborhoods.
Reduced access to preventative healthcare services.
Limited educational and employment opportunities.
These disparities are often the result of structural factors, including historical policies, systemic inequality, and uneven resource distribution.
Why Community-Based Solutions Matter
Traditional healthcare models focus primarily on treating illness after it occurs. However, improving health equity requires addressing the upstream factors that shape health long before a patient enters a clinic or hospital.
This is where community based organizations play a critical role. We take a community-centered approach and recognize that health is interconnected with education, opportunity, and social support. This organization works to empower communities by addressing both immediate needs and long-term structural challenges.
Moving Toward a More Equitable Future
Improving health equity is not a simple or quick process. It requires collaboration across sectors including public health, education, housing, transportation, and economic development. But meaningful progress begins with awareness.
Understanding how social determinants influence health can change how we think about healthcare itself. Instead of focusing solely on treatment, communities and policymakers can invest and must in prevention, opportunity, and equity.
Community organizations like our own demonstrate how local initiatives can play a powerful role in advancing this mission. By connecting education, advocacy, and community engagement, we help create environments where individuals have the tools and resources needed to thrive.
When we improve the conditions in which people live, learn, and work, we improve health for everyone.
Resources to Learn More
If you want to explore health equity and social determinants of health further consider these resources.
Centers for Disease Control and Prevention - Social Determinants of Health
World Health Organization - Social Determinants of Health
Office of Disease Prevention and Health Promotion - Healthy People 2030